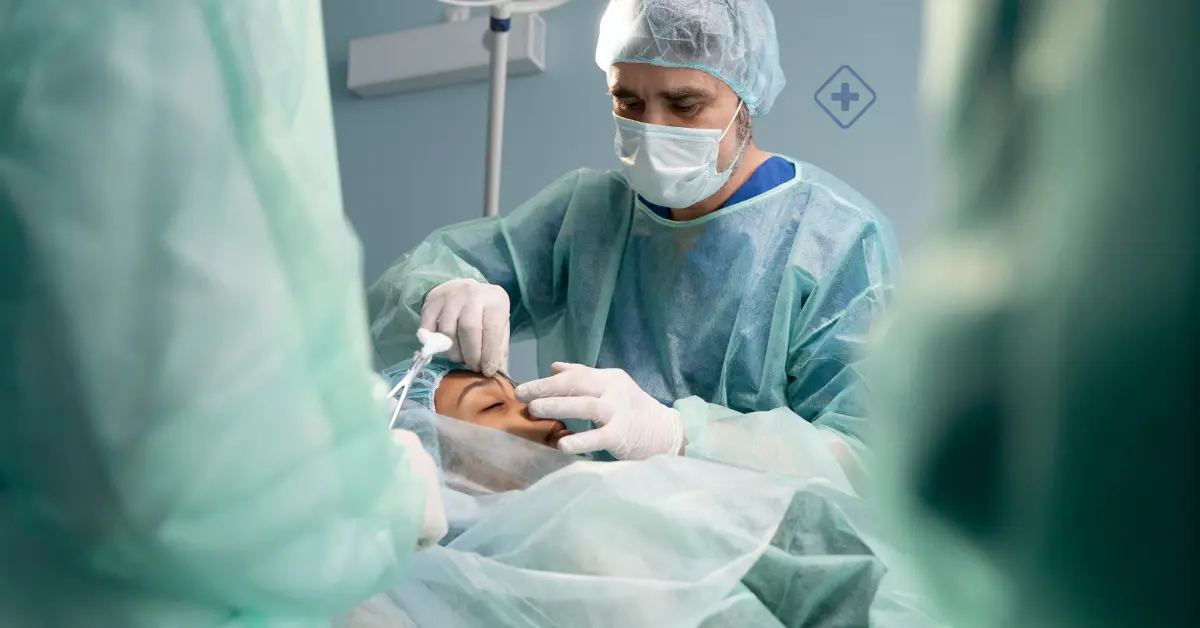
Inside the Intensive Care Unit: What's going on? What to Expect?
The intensive care unit (ICU) is dedicated to the care, monitoring and assistance of patients suffering from serious illnesses.
.jpg?q=HQJukfHlUEuslnir)
What is an Intensive Care Unit?
The ICU is oriented to the care, monitoring, and assistance of patients with life-threatening or emergency medical conditions, such as serious injuries, accidents, severe respiratory problems, and acute illnesses and infections, which are life-threatening.
The difference between the ICU and other hospital wards is that:
-
Care and monitoring are provided 24 hours a day by a team of specialists, nurses, medical assistants, therapists, etc., who are highly trained to do their job.
-
The number of beds is much smaller, but the medical team of monitoring and care is greater
-
Visits are more controlled
The staff working in the Intensive Care Unit (ICU) area is aimed at stabilizing the patient's vital signs. Providing support measures for organ and system failures that may occur.
Intensive care involves close monitoring of the patient's signs and general condition with advanced care at the neurological, hemodynamic, respiratory, nutritional, metabolic, and hydrolytic levels, supported by the imaging services and clinical analysis laboratory to perform the necessary studies for each case.
Many teams have alarms and flashing lights, which help health personnel supervise patients and do not mean that something is wrong.
When is a patient required to enter the ICU?
To send a patient to the Intensive Care Unit, there are very specific criteria; that is, after evaluating the patient's general condition, stability, vital signs, among other possible complications, the Intensive Care Physician may point out that the patient needs IC, when any of the following situations occur, which are usually the most common:
-
Severe lung problems or respiratory failure
-
Problems with serious infections (Example: Sepsis, Pneumonia)
-
Serious accidents or injuries such as car accidents, shootings or falls
-
Severe burns
-
Severe bleeding
-
Patients recovering from major surgery
-
When a baby is born with a severe illness or prematurely, this unit is called the Neonatal Intensive Care Unit (NICU)
What precautions should I take when visiting someone in the ICU?
Visitors to each ICU have different policies, so approach someone who can give you more specific information about the Hospital where your family member or loved one is. Generally, visitors in this area are allowed only to the patient's immediate family.
When visiting someone in the ICU, consider that people with serious illnesses or sensitive causes are in this area:
-
Wash your hands thoroughly and apply any other safety and hygiene measures indicated (for example, put on a gown, face mask and/or a headcover, which are not always necessary but in some cases, the staff will ask you to do so)
-
Preferably turn off your cell phone
-
Avoid carrying gifts or flowers (as these can carry spores that cause infection). Remember that infection control is critical for patients who are very sick and have a weakened immune system
-
If you think you might have a disease such as a cold or something that could be contagious, please postpone your visit
Techniques and Procedures that are carried out within the ICU:
If a family member or loved one has been admitted to the Intensive Care Unit, you may feel confused about what procedures will be performed or what happens there. It all depends on the patient's specific health condition and the cause for which he or she is in this Unit. However, some of the techniques and procedures that could be applied to him or her are:
-
Catheters and/or drains:
On admission and during the stay in the ICU, the patient is given catheters as a means of administering medication and the extraction of blood tests.
Also, depending on the patient's needs, drains may be applied.
Drains are tubes placed in different parts of the body, such as the abdomen, head, or chest, and used to remove fluids or air if necessary.
-
Intubation:
This refers to the technique of placing a tube through the mouth into the lungs to help the patient breathe. To do this, the patient is given anesthesia, then connected to a ventilator and given medication.
There are situations when your family member or loved one needs to be sedated or "asleep" for several days. Remember that while he is intubated, he will not be able to talk.
-
Ventilator:
With this technique, a special ventilator connected to a mask covering the nose and mouth delivers air and oxygen to the lungs. During this procedure, the mask needs to be tightly fitted to the face so that the air does not escape.
-
Tracheotomy:
A tracheotomy is a small surgical procedure where, after the patient has been anesthetized, an air passage is created to allow breathing when the standard breathing path is reduced or obstructed. This is done by inserting a temporary tube into the trachea that reaches the lungs to help the patient breathe.
A tracheostomy is usually temporary, providing an alternative to the regular breathing path until other medical problems are resolved. If the patient needs to stay on a ventilator indefinitely, a Tracheostomy is usually the best permanent solution.
Other procedures that can be seen within the ICU are:
-
Placement of a permanent intravenous pacemaker
-
Post-operative management of cardiac surgery
-
CPR maneuvers
-
Renal Replacement Therapy
-
Pediatric Intensive Care
-
Hemodynamic support
What to expect?
You can feel safe and confident that the medical team's priority in charge of the ICU area is always to care and assist the patient in the best way. Therefore, your patience and understanding are greatly appreciated during these emergencies that we know are not easy.
It is possible that situations of confusion and disorientation may arise as your family member or loved one wakes up. The application of sedatives and anesthesia, other medications, disorganized sleep schedules, among other factors that contribute to the patient having no sense of time and not remembering where he or she is or if it's day or night, among other things.
For many family members, the fact that the patient leaves the Intensive Care area can be a factor of joy and happiness as for others it can be a reason for anxiety because thoughts such as "he should stay here until he returns to normal completely" or "and what happens if he gets worse" come to mind. Still, the medical staff in this Unit has the expertise to determine if a patient's condition is stable.
Some patients may be sent to complete their recovery directly to their homes; others must spend more time in a regular room in the Hospital area to continue their control and monitoring, which, although less intense, is just as necessary. This step is an important event on the road to recovery because it means that the patient no longer needs intensive therapy.
BlueNetHospitals - Hospital Los Cabos
BlueNet Hospitals.
Trending Topics
Pregnancy infections (TORCH)
Risks, testing, and prevention
Anemia in Women of Reproductive Age
Symptoms, Causes, and Prevention
Head and Neck Surgical Oncologist: The Key Specialist in Your Diagnosis
Discover what they do, which conditions they treat, and when it’s important to seek an evaluation.
Newborn Metabolic Screening: The Test That Helps Detect Diseases from the First Days of Life.
Learn what newborn screening is, when it should be performed, and why it is a fundamental test for the early detection of diseases in newborns.
Health Library
ICU
- Do You Need an Appointment with a Specialist?
- call us
- write us
- let's talk