Rheumatoid Arthritis
Rheumatoid Arthritis (RA) is a chronic, autoimmune disease primarily affecting the joints, resulting in inflammation.

Rheumatoid Arthritis (RA) is a chronic, autoimmune disease primarily affecting the joints, resulting in inflammation and damage. Although the exact cause of rheumatoid arthritis remains unknown, it's believed that a combination of genetic and environmental factors significantly contribute to its onset.
The disease can significantly impact the quality of life of those suffering. However, with proper diagnosis and treatment from a rheumatologist, it's possible to manage its symptoms and minimize long-term complications.
What are the symptoms of Rheumatoid Arthritis?
The symptoms of RA can vary in intensity, and manifestation tends to affect the joints symmetrically—meaning if one joint of a hand or foot is affected, likely, the other is too. Common symptoms include:
-
Joint pain: Feeling pain, stiffness, and tenderness in the joints, often in the morning or after periods of inactivity.
-
Swelling and warmth: Affected joints may be swollen, red, and feel warm to the touch due to inflammation.
-
Morning stiffness: Many people with RA experience prolonged joint stiffness upon waking, lasting longer than an hour.
-
Fatigue: RA can provoke a generalized feeling of tiredness and fatigue, not always related to physical activity.
-
Loss of mobility: In time, chronic inflammation and joint damage can lead to a loss of mobility and affect the ability to perform daily activities.
-
Rheumatoid nodules: Some people with RA may develop small lumps under the skin, known as rheumatoid nodules, which tend to appear in areas exposed to pressure, like elbows.
Complications of Rheumatoid Arthritis
Untreated or poorly managed rheumatoid arthritis can lead to serious complications that affect various body systems. Some of the most common complications include:
Joint damage and deformities
Chronic inflammation can lead to cartilage and bone erosion in the joints, causing deformities and loss of function.
Lung problems
RA can affect the lungs, causing inflammation in the lung tissue and increasing the risk of interstitial lung diseases.
Cardiovascular diseases
People with RA are more likely to develop cardiovascular diseases like heart disease and stroke.
Sjögren's syndrome
Some people with RA may also develop Sjögren's syndrome, which affects the glands, producing tears and saliva, causing dryness in the eyes and mouth.
A rheumatologist should always accompany an RA diagnosis to prevent complications and maintain optimal quality of life.
People Prone to Rheumatoid Arthritis
Although RA can affect anyone, there are risk factors that can increase the likelihood of developing the disease:
-
Genetic factors: Family members with a history of rheumatoid arthritis can increase one's predisposition.
-
Sex: Women are more likely to develop rheumatoid arthritis than men.
-
Age: RA can occur at any age, but it's more common in people between 40 and 60.
-
Smoking: Cigarette smoking increases the risk of developing rheumatoid arthritis, especially in people with a genetic predisposition.
Treatment for Rheumatoid Arthritis
The aim of treating rheumatoid arthritis is to control the symptoms, prevent joint damage, and improve the patient's quality of life. Here are some approaches a rheumatologist might take to manage this disease:
Medication
Doctors may prescribe medication to reduce inflammation, relieve pain, and slow disease progression. These include non-steroidal anti-inflammatory drugs (NSAIDs), corticosteroids, disease-modifying antirheumatic drugs (DMARDs), and tumor necrosis factor (TNF) inhibitors.
Physical therapy and exercise
Physical therapy and professionally supervised exercise can help maintain mobility and strengthen the muscles surrounding affected joints.
Lifestyle changes
Following a healthy diet, maintaining proper weight, and avoiding smoking can positively impact managing the disease.
Complementary therapies
Some people find relief with complementary therapies like acupuncture, mindfulness meditation, and yoga.
It's vital for individuals with rheumatoid arthritis to work closely with their medical team to develop a personalized treatment plan and adjust it as needed.
Visit BlueNetHospitals, where our specialists will provide help from the first consultation in monitoring and treating rheumatoid arthritis.
BlueNetHospitals - Hospital Los Cabos
BlueNet Hospitals.

Influenza
The symptoms of influenza are similar to those of other respiratory infections but tend to be more intense
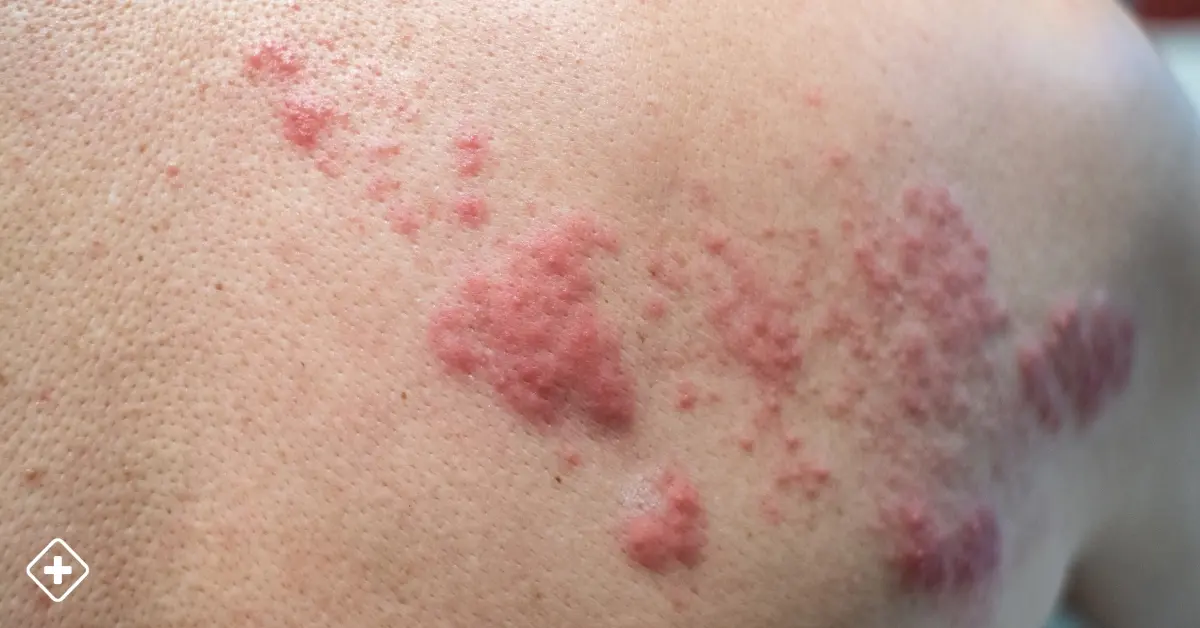
Shingles
Shingles, also known as herpes zoster, is a viral infection caused by the varicella-zoster virus responsible for chickenpox
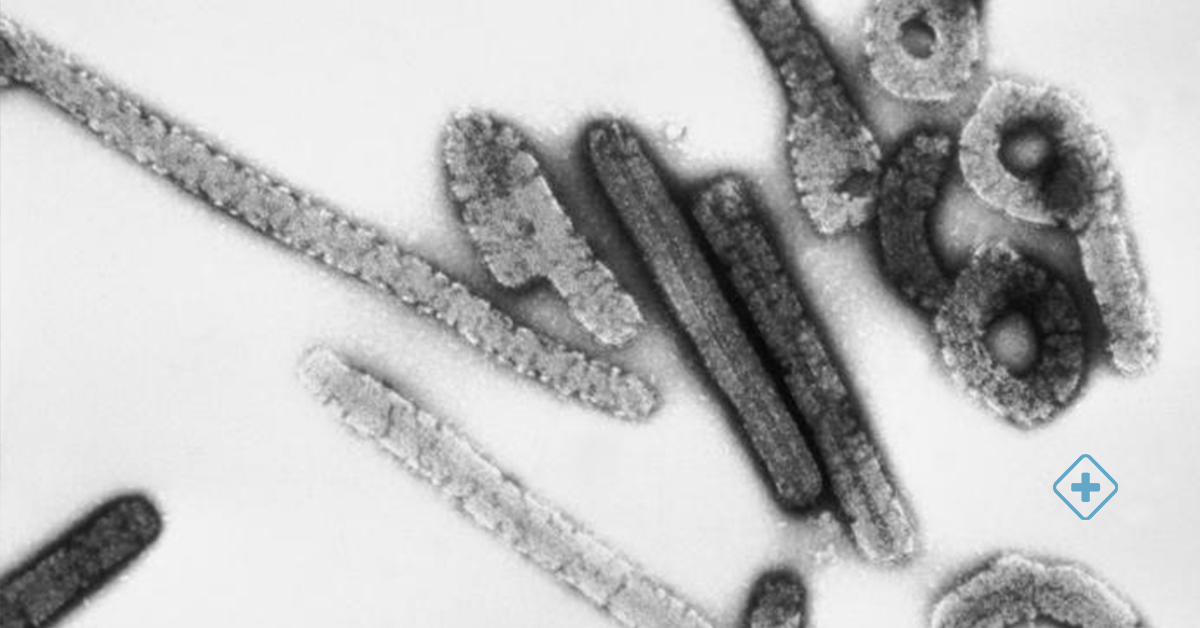
Marburg Virus
What is the Marburg Virus? How is it spread? What are the causes?
- Do You Need an Appointment with a Specialist?
- call us
- write us
- let's talk