Coronary Artery Disease
Coronary artery disease occurs when the blood vessels supplying your heart are damaged. Cholesterol in the coronary arteries and inflammation are usually the first causes.

¿What is Coronary Artery Disease?
Coronary arteries are those that carry blood with oxygen to our hearts.
When these arteries are obstructed by the accumulation of fatty deposits inside them and unable to supply the heart with blood adequately, it is known as Coronary Artery Disease. If the heart is not getting the blood and oxygen it needs, it can cause chest pain (Angina), Arrhythmia, or Heart Failure.
The build-up of this plaque of fat, cholesterol, and other substances in the heart's arteries can even lead to a Heart-Attack, resulting in permanent heart damage. This is the most common disease as well as, unfortunately, the most significant cause of death in both men and women in the USA.
Causes of Coronary Artery Disease
Following are some of the possible causes:
-
Smoke
-
Physical inactivity
-
Insulin resistance
Symptoms of Coronary Artery Disease
Symptoms regularly vary from person to person. Over time, as the arteries become blocked, it can appear:
-
Chest discomfort or pain (Angina)
-
Breathing difficulties
-
Tension or several pains in the arms, shoulders, neck, jaw, and back
-
Fluid retention in the feet
-
Extreme tiredness and fatigue after exercise
-
Excessive sweating
-
Nausea
-
Cramps
-
Weakness
-
Shortness of breath from any form of physical activity because the heart is not getting enough oxygen
Risk Factors for Coronary Artery Disease
-
Strong family history of heart disease
-
High cholesterol
-
Excessive alcohol and cigarette consumption
-
Diabetes or insulin resistance
-
Sedentary lifestyle
-
High stress
-
Age: As we get older, the risk of damage to our arteries increases
When you have two or more risk factors, your risk of coronary artery disease is higher. If you know or feel that you have any of these symptoms or risk factors, do not hesitate to discuss them with your Cardiologist. He/she will most likely recommend you undergo some tests to detect or discard Coronary Artery Disease.
Diagnosis of Coronary Artery Disease
There is no unique test to diagnose Coronary artery disease because several factors play a role. Your Cardiologist will likely perform a physical exam, listen to your heart, and ask you some questions about your lifestyle, family history, and medical conditions that will determine if there is a need to order more tests to detect or rule out Coronary Artery Disease.
Some of the most common studies are:
-
Electrocardiogram: It records the electrical activity and rhythm of the heart; an EKG may reveal evidence of a previous or ongoing heart attack.
-
Holter monitor: A portable device is placed under your clothing for 1–2 days to monitor your heart's activity while you go about your daily activities.
-
Stress test analyzes how the heart works before and after a physical effort. The Cardiologist will put you on a treadmill or stationary bike or give you some heart-boosting medication.
-
Blood tests: Usually used to measure and monitor blood cholesterol levels
-
Echocardiogram: An echocardiogram determines if all heart parts naturally contribute to the heart's blood and oxygen pumping by using sound waves to produce images of the heart organ.
Treatment of Coronary Artery Disease
The first thing to consider is that if you already know that you have Coronary Artery Disease, you have to learn to be aware of the potential risk, and it is under your control to reduce it.
-
Diet, exercise, and quitting smoking are some examples.
-
Your body may need more time to make noticeable progress, so your doctor will monitor your progress and tell you what medications can help control this condition.
-
Cholesterol-modifying medications: Your cardiologist will tell you if and which ones to take. These medications reduce plaque in the coronary arteries, especially bad cholesterol (LDL).
-
Beta-blockers lower blood pressure and slow the heart rate. They are especially recommended for people who have had a heart attack in the past.
-
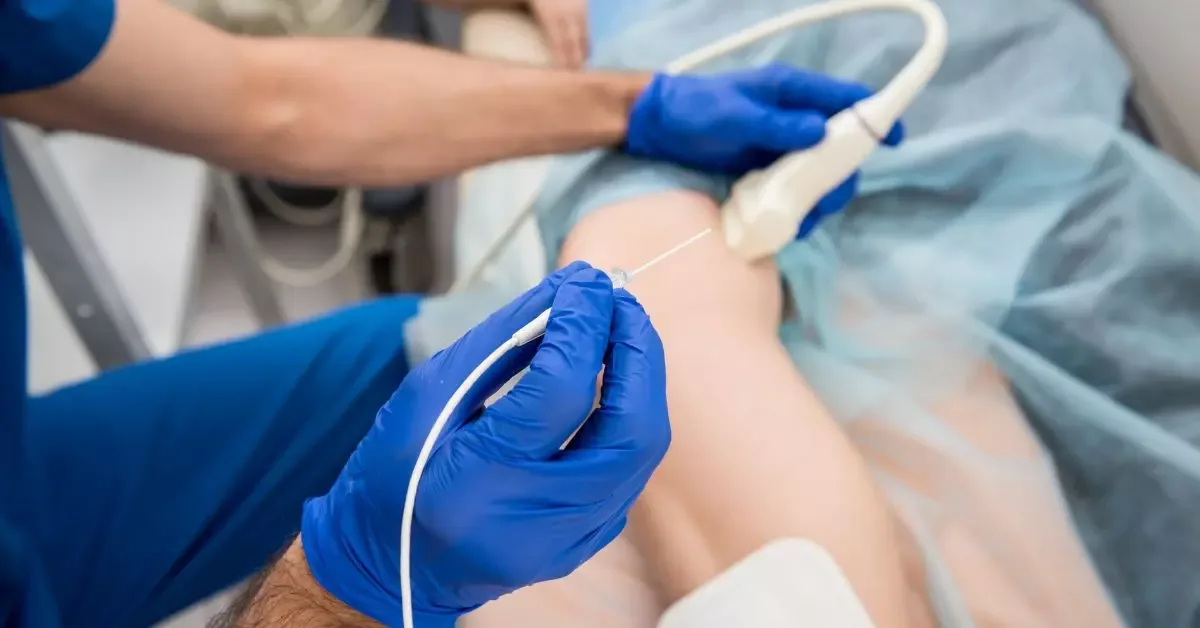
Angioplasty: This procedure restores blood flow through the narrowed artery. The Cardiologist inserts a catheter with a small balloon on one side. Once in place, the balloon is inflated to push the plaque against the artery wall, thus widening the artery.
-
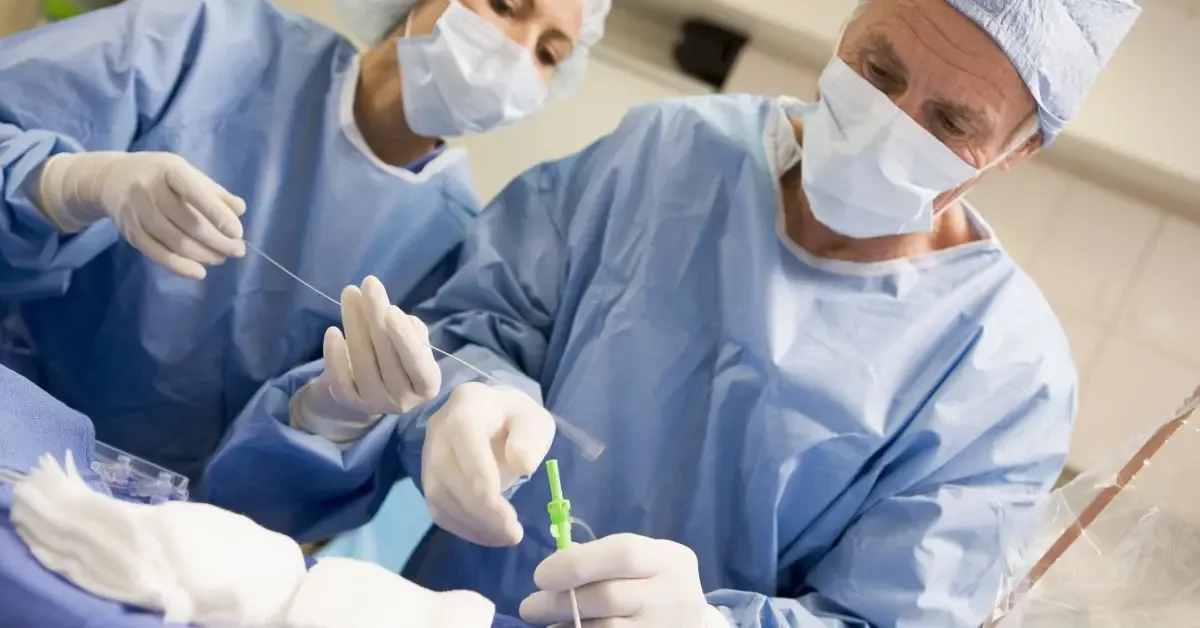
Coronary Artery Bypass Surgery: The specialist surgeon creates a graft using a blood vessel from another body part to bypass the blocked coronary arteries.
You must consider regular check-ups with your cardiologist because early detection of coronary artery disease is fundamental to preventing more severe consequences.
Living with Coronary Arteries Disease
When you have already been diagnosed with Coronary Artery Disease, follow the treatment provided by your Cardiologist.
Some things to consider that could help improve the quality of life are:
-
Find out about your illness
-
Eat healthily
-
Do not smoke
-
Attend your appointments with the Cardiologist
-
Take the medications provided by your Cardiologist
-
Do regular and continued exercise
¿When do you have to see a doctor?
If you present any of the mentioned symptoms or detect another abnormal sign, go to the Cardiologist.
When consulting your Cardiologist, try to keep a record of your pain with a detailed description of the symptoms, duration, and what you think triggered them. Also, mention any medications you are taking.
BlueNetHospitals
BlueNet Hospitals Blue Net Hospitals

Cardiac Ablation: Treatment for Atrial Fibrillation and Arrhythmias
Cardiac ablation is recommended when treatments are no longer effective or are not well tolerated to treat arrhythmias
Extrasystoles
Ventricular extrasystoles may not present symptoms; in other cases, they may cause unpleasant or alarming sensations.
Heart Murmurs: Symptoms, Causes, Diagnosis and Treatment
Heart murmurs are abnormal sounds heard during a heartbeat as blood flows through the heart valves or chambers. Learn about symptoms, causes, diagnosis, treatment options, and when a heart murmur may signal an underlying cardiovascular condition.
Cardiac Catheterization: Diagnosis, Treatment, and Coronary Artery Evaluation
Cardiac catheterization is a specialized procedure used to diagnose and treat cardiovascular diseases by evaluating coronary arteries, heart valves, blood flow, and overall heart function.
- Do You Need an Appointment with a Specialist?
- call us
- write us
- let's talk